
UM Shore Regional Health Center – Chestertown
Small rural hospitals are an endangered species everywhere in the U.S. In Kent County, an intense, citizen-led campaign to save the Chestertown hospital has made progress, but—contrary to recent press reports—the hospital’s fate is still uncertain. Shore Regional Health, part of the University of Maryland Medical System that provides healthcare to 5 mid-shore counties and which owns and operates the Chestertown facility, has said it would like to maintain in-patient services in Chestertown after 2022, as part of a broader plan to upgrade healthcare on the Eastern Shore. But doing so will be contingent on legislative or regulatory changes to establish a new reimbursement model for vulnerable rural populations. Whether such legislation is passed is likely to depend on recommendations in the upcoming report of the Maryland Rural Health Study, due this September. Watch this space for an in-depth report when the recommendations are released.
But the future of the hospital—as a full in-patient facility or as a standalone medical facility with more limited services—is only one of the factors that are likely to shape healthcare in the county in coming years. Moreover, a just-released nationwide assessment of the quality of health—county by county within each state—finds that Kent County has lots of room for improvement. It ranks only 18th (out of 24 Maryland counties) in health outcomes, far behind Talbot (5th) and Queen Annes (7th), and only barely ahead of Caroline and Dorchester.
Healthcare is changing rapidly, driven by both economic pressures (healthcare expenditures make up nearly 20% of the U.S. economy, far above all other industrial countries) and by new technology. Shore Health’s strategic plan for the Eastern Shore deals with both aspects, but focuses on improving access to care, while also implementing services that can help keep people out of hospitals. Here we profile some technologies and other innovations likely to impact our healthcare in one form or another in coming years, drawing on both local and national examples.
Transport. A big unmet need in Kent County, as in most rural areas, is transport to get people to care. That could take the form of local transport—to see a doctor, then pick up medicines at a drugstore—or could mean emergency transport by van or helicopter to a distant hospital. One model for local transport could be a kind of “Uber for healthcare” service that would allow people without cars or who can’t safely drive to arrange pickup and transport when they need it with just a phone call or an app. Potentially, a similar service—private but subsidized, or run by a healthcare system or insurer—could also provide transport services to regional hospitals. Will any of these happen? Such services are being started or are under discussion in a few places already, but whether they happen here may depend on local initiatives and some state financing.
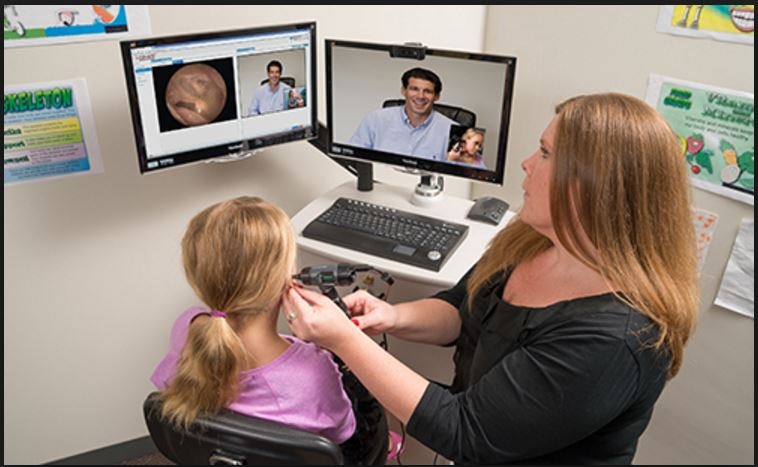 Telemedicine and Telehealth. Under the best of circumstances, however, it’s a hassle to drive across the bridge to consult a surgeon or a specialist not found on the Eastern Shore. Suppose instead you could talk to them over a video link from a local facility or, eventually, even from home? As it happens, Shore Regional Health is already gearing up for telemedicine services on the Eastern Shore, in part under a grant from the Maryland Health Care Commission. In April the first patient, a 22-month old boy brought to the emergency room at the Easton Hospital, was linked in minutes to a specialist at the University of Maryland Medical Center in downtown Baltimore—resulting in a diagnosis, immediate treatment, and referrals for followup. “Bridging the gap between the eastern and western shores is a wonderful opportunity that this technology has given us,” says Marc T. Zubrow, MD, vice president of telemedicine for the University of Maryland Medical System. “We will continue to enhance and expand the telemedicine capabilities [to] allow patients to receive the expert care they need without having to leave their local communities and support systems.”
Telemedicine and Telehealth. Under the best of circumstances, however, it’s a hassle to drive across the bridge to consult a surgeon or a specialist not found on the Eastern Shore. Suppose instead you could talk to them over a video link from a local facility or, eventually, even from home? As it happens, Shore Regional Health is already gearing up for telemedicine services on the Eastern Shore, in part under a grant from the Maryland Health Care Commission. In April the first patient, a 22-month old boy brought to the emergency room at the Easton Hospital, was linked in minutes to a specialist at the University of Maryland Medical Center in downtown Baltimore—resulting in a diagnosis, immediate treatment, and referrals for followup. “Bridging the gap between the eastern and western shores is a wonderful opportunity that this technology has given us,” says Marc T. Zubrow, MD, vice president of telemedicine for the University of Maryland Medical System. “We will continue to enhance and expand the telemedicine capabilities [to] allow patients to receive the expert care they need without having to leave their local communities and support systems.”
Telehealth refers to broader, non-emergency services at a distance, linking patients at home to doctors or nurses via voice or video or data links. A patient with high blood pressure at risk for stroke, for example, might periodically measure his or her blood pressure at home with a device that transmits the data to be screened automatically by an algorithm and checked periodically by a nurse. Many wearable or in-home sensors capable of monitoring chronic health conditions are now available. Telehealth calls or data streams can also record physical exercise, help patients to improve their nutrition, help a mother decide whether her baby’s fever is high enough to need a doctor’s care, or address other health concerns. The savings in costs and peace of mind could be substantial, and sometimes life-saving.
In-home Care. Some health conditions call for personal contact by a nurse, physical therapist, or health coach. Increasingly, taking care to the patient at home is not only less expensive than institution-based care, but sometimes far more effective—as well as overcoming the necessity to travel and the tendency to put off seeking care. Surgical aftercare through home visits is now common, in-home infusions or dialysis or massage therapy constitute a growing trend. Regular visits by a nurse or a health coach, especially for seniors with chronic conditions or for those struggling with opioid and other addictions, are being tested or considered in many places, and there is some evidence that such visits are more effective in helping people adopt healthy behaviors than care in an institutional setting—as well as less expensive. Assistance with non-medical tasks of daily living that are important to maintaining health are now often provided by volunteers, but increasingly such wellness services are being viewed as a part of basic healthcare. In one instance in California, simply inspecting homes of seniors and installing grab bars or stair railings or replacing loose rugs cut the number of falls (and the resulting hospital stays) in half.

The Amazon Dot, a smaller version of the Amazon Echo, can help with daily tasks, make phone calls, answer questions, even remind a person to take medication at a certain time.
A Virtual Health Coach. Millions of people now have an Amazon Echo and its voice-driven intelligent assistant, Alexa, that they use to order new supplies, turn on lights, or play music—just by talking to it. Now Alexa (and similar voice-based systems from Google and Apple) are starting to be used in healthcare. Alexa can answer questions about your conditions or symptoms or an upcoming doctor’s appointment, remind you to take medicines or order refills, or provide updates on vital signs or pain levels to a remote nurse—all without touching a computer. If you fall, Alexa can call the ambulance. For patients with limited eye sight or who are bed-ridden, Alexa can become a constant companion and a vital link to assistance.
Expert Assistance. Increasingly, large organizations are using artificial intelligence tools to mine large datasets and “learn” how to do things more effectively. So as voice-driven systems interact with millions of patients, asking them about their symptoms—and that data is coupled to the clinical signals provided by in-home sensors for blood pressure, blood sugar, fever, etc.—it’s not very far fetched to imagine that IBM’s Watson or other AI systems may be able to diagnose many health conditions as well as even the most expert doctors—and enable earlier diagnosis and treatment—all without leaving home.
If such things seem hard to imagine, remember that Kent County will soon have the essential infrastructure—near universal access to fast internet connectivity. Keeping in-patient services at the hospital would be important (and might take some lobbying with lawmakers in Annapolis). But in the long run, improved access to care through the new tools and services described above, especially for vulnerable populations, may be even more important for the future of health than what kind of local health facility we have.

The Amazon Echo with “Alexa,” your new personal – and maybe even healthcare – assistant.
###



Karen P O'Connor says
The author makes several interesting points and describes many things that are going to be a part of our healthcare environment . In the near term, we still have unresolved issues with transportation. This has been a part of the discussion on healthcare in Kent County now for well over 10 years and no one seems to be willing or able to address it. I found it interesting that universal access to high speed internet is equated with actually being able to afford to hook up and use it. Here is the conundrum of rural healthcare delivery. Providing “access” does not equate to providing badly needed services to those that need them. It is as much an economic issue as a time/distance one. I look forward to seeing in concrete terms how the problems of access will be addressed in the fall report.
Stuart Elsberg says
Mr. Hammond’s article has obviously been extensively researched. I would like to add a few notes to his broad presentation. First would be that Telemedicine linking the Shore Medical Center in Chestertown to the University of Maryland Medical Center in Baltimore (and its staff of specialists) has been in use for several years. Secondly, as concerns linking vulnerable citizens to home assistance services, or helping to make home environments safer for that population, were integral to the mission in the founding of Home Ports in Kent County. (Note–The Spy has run articles and interviews about HomePorts many times.) This is in addition to the Shore Regional’s Chester River Home Care home health staff that has visited and cared for chronically ill patients at home since the 1990’s.
I commend the Spy on continuing to focus on the health care services we do have, and that maintaining (and, hopefully, growing) those services depemds on vigilence and activism by all of us in the community.
–Mickey Elsberg