As the Mid-Shore’s UM-Shore Regional Health starts to finalize reorganization plans this fall, including the future role of health care in Chestertown, Cambridge, and Easton, the Spy thought it would be interesting to understand more clearly the economic forces at play that required organizational reconstruction in the first place.
And on that question, we could find no better place to turn to than Maryland’s Health Services Cost Review Commission, or affectionately known as HSCRC. While the name might sound bureaucratic and even rather benign, the truth is that the HSCRC is at the heart of a revolutionary change taking place on the Eastern Shore and every other region in the state.
Why? It is because this tiny state agency, located next to a Burlington Coat Factory and a Panda Express near Baltimore, single-handedly decides the rates and global budgets for hospital services located at a hospital – for both inpatient and outpatient services. In other words, it doesn’t matter who pays your medical expenses, private health insurance, Medicare, or Medicaid, those charges only exist with the full approval of the HSCRC. It’s a big deal.
In fact, Maryland is the only state in the country that can control significant aspects of its health economy. And while it has been able to set health care costs since 1977, it was only in January of 2014 that the HSCRC instituted a new “All Payer” model that permanently terminated its pay for services model.
The end of pay for services has been replaced by a revenue model that encourages and economically rewards health systems that appropriate care options beyond inpatient care. At the same time, that same model pushes regional hospitals to increase community health programs that dramatically reduce the need for inpatient care with those with chronic illnesses.
Sitting on top of this revolution is Donna Kinzer, HSCRC’s executive director. A health policy consultant and analyst for several decades prior to joining HSCRC, her passion for redefining health care comes from a personal family tragedy. While caring for her terminally ill husband when she was 39 years old, Donna witnessed first hand how the old “hospital door to hospital door” model was grossly inadequate for both the patient and as a sustainable business model.
This video is approximately fourteen minutes in length
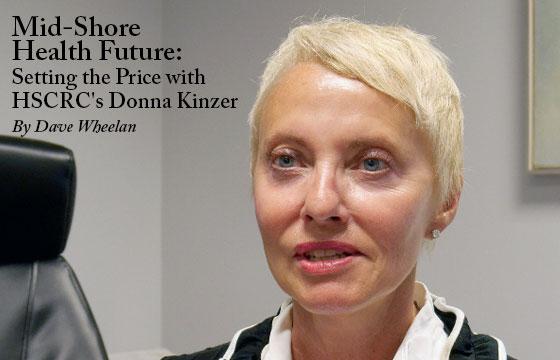


Stephan Sonn says
Ms Kinzer is a very concerned professional and we are fortunate to have her in Maryland.
Her parsing was indeed minimal and her concerns most compassionate.
However UMMS may habe a game plan that will seem to conform with her broad outline, but not to Chestertown’s preferences.
Let me give you what could be a well positioned UMMS strategy model from the cherry picking school of hospital future planning.
Dumping Chestertown and then reassigning space in an Easton sub hub by pumping up favored specialties
with big ticket designer super pavilions as part of a geriatric grid covering our part of the Eastern Shore.
It has already started, holding to a for profit model well set to the original intentions.
Going with the money. Perhaps more deftly called designer medical pavilions.
Musical chairs, odd man out maybe for Chestertown, but lots of bragging rights for UMMS.
Karen O'Connor says
While some interesting general information is presented, I did not hear anything that helps to explain in plain dollars and cents what our regional healthcare system is facing from HSCRC, and how it impacts the distribution of services here on the mid and upper Shore. Being able to manage chronic disease using outpatient and preventive services will take many years to show substantial results in reduced admissions. Some conditions, such as congestive heart failure, are exceedingly hard to manage on an outpatient basis, yet hospitals are penalized severely for re-admission within a set time frame for a specific condition. This type of information would be more meaningful and help non- health care people understand what Ms. Kinzer is describing. More specifics, please!
Stephan Sonn says
The reason that there are no specifics is that it is all still on the fly. At the moment the clock is counting down on the emergence of “actuarial healthcare.”
Whereby the shark may get jumped and that is the bad news. That is not so hard to understand, granting that this all may be an unholy marriage of compassion and constriction. Try that!